Dynamic Body Surface Analysis for Functional ACL Assessment: An innovative perspective
20 December 2025.
Autor/es: Salvador Pitarch Corresa, Fermín Basso Della Vedova, Paqui Peydro De Moya, Juan López Pascual, Eduardo Pérez Bocanegra*.
Instituto de Biomecánica (IBV)
Anterior Cruciate Ligament (ACL) injuries currently remain a challenge that requires exhaustive functional evaluation to guarantee recovery and prevent future re-injuries. In this context, dynamic body surface scanning technology (MOVE4D) emerges as a highly valuable and innovative tool in biomechanical analysis. This system is crucial because it allows for the quantification of the body’s three-dimensional morphology in motion, offering a unique perspective by combining morphological, kinematic, and functional metrics. The study of dynamic morphology provides vital information on structural variables (such as atrophy or edema) and functional variables (soft tissue deformation). In this way, dynamic morphological analysis enhances the precision of post-ACL assessment and guides more objective decisions regarding functional progression
INTRODUCTION
Anterior cruciate ligament (ACL) injuries of the knee are currently considered one of the most common pathologies both in sports and in the general population. They frequently occur during movements that involve jumping, pivoting, or sudden changes of direction, whether in sports or work settings, and are often associated with physical exertion, movement on uneven surfaces, or work-related accidents.
These injuries typically lead to alterations that affect the biomechanics of the knee and the functional capacity of the lower limb. Therefore, proper assessment and follow-up of this injury are essential not only for returning to sports but also for regaining adequate function in daily or work-related activities.
In this regard, it is not sufficient to assess only the integrity of the ligament reconstruction. Dynamic evaluation through movement patterns is essential, as well as monitoring of the musculature to ensure a safe return, with the goal of reducing the risk of re-injury or joint degeneration. There are examples in the literature [1,2] that highlight morphological and physiological changes—such as reductions in strength and modifications of cross-sectional area and muscle volume—as long-term negative effects of ACL injuries.
Several studies have shown that, after an ACL injury or reconstruction, gait kinematics may approach a nearly symmetrical pattern between the affected and contralateral limbs, especially in advanced stages of recovery. However, this apparent normalization of joint kinematics does not imply a complete restoration of muscle function [3,4].
In routine clinical practice, follow-up after ACL reconstruction continues to rely mainly on time-based criteria to estimate recovery, complemented by strength and functional tests, as well as instrumental biomechanical assessments. Currently, when assessing and monitoring ACL injuries through motion-capture technologies (3D stereophotogrammetry, IMUs, and markerless systems) information on joint kinematics is obtained, but this is influenced by limitations such as soft tissue artifact, sensor drift/placement, and accuracy that varies depending on the task and the population. On the other hand, in muscle assessment, surface electromyography is sensitive to crosstalk and electrode placement despite existing guidelines for its standardized use. All these factors may influence, to a greater or lesser extent, the reliability and accuracy of these analyses.
DYNAMIC BODY SURFACE SCANNING: MOVE4D, WHAT IT IS AN WHAT IT PROVIDES
This highlights the need for methodologies and evaluation systems that go beyond recording muscle activity or studying joint kinematics, incorporating morphological variables in both static and dynamic ways during functional movements.
Dynamic body surface scanning allows the visualization and quantification of changes in body geometry during movement, capturing the differences between static and dynamic postures. This technology can reveal how the body surface and its measurements are altered with movement, which is valuable for understanding movement-related changes in body shape [5].
The MOVE4D dynamic body surface scanning system, combined with automated processing software, enables the generation of watertight and homologous digital human models. This homologous mesh, composed of 50k vertices, maintains a one-to-one correspondence throughout the entire temporal recording, thus allowing reproducible analysis of these metrics.
Therefore, the use of MOVE4D offers direct and repeatable quantification of perimeters, areas, and volumes of body segments, making it possible to detect objective surface changes related to atrophy, edema, and muscle activity [6]. Additionally, the information extracted from the homologous mesh enables reliable and accurate markerless calculation of joint kinematics [7,8].
MOVE4D allows these metrics to be obtained in a simple, fast, and automated manner both statically and dynamically, during functional tasks or positions, representing a distinctive innovation.
This technology, in addition to obtaining joint kinematics without the need to instrument the subject, can provide several advantages such as:
- Objectively quantifying muscle atrophy or the recovery of muscle volume.
- Analysing morphological symmetry between limbs during movement.
- Evaluating how the morphology of a body segment changes in specific phases of a functional movement.
The aim of this article is to describe the innovative contribution of dynamic surface scanning in the monitoring of ACL injuries, highlighting its potential to enhance the precision of functional assessment. To this end, a case study is presented involving a subject 3 month post-surgery for ACL and lateral meniscus in the right knee, who exhibits altered muscular trophism in the limb, primarily affecting weight-bearing movements.
DESARROLLO
A static study and assessments of gait and semi-squats were carried out using the MOVE4D system with the objective of:
- Obtaining joint kinematic data to determine movement functionality.
- Studying possible structural asymmetries through the static assessment of body segments.
- Identifying possible alterations in muscle function through the dynamic analysis of soft tissue behaviour.
The variables extracted from the study are:
- From the static assessment: the perimeter of the mid-thigh and the knee.
- From the dynamic assessment: knee angles; perimeters of the distal third of the thigh and the upper third of the leg; and segmental volumes of the thigh and leg for each gait cycle and semi-squat movement.
resultads and interpretation
I. KINEMATIC ASSESSMENT OF GAIT AND SEMI-SQUAT
First, kinematic information was extracted through the mesh to help interpret the results of the morphological analysis.
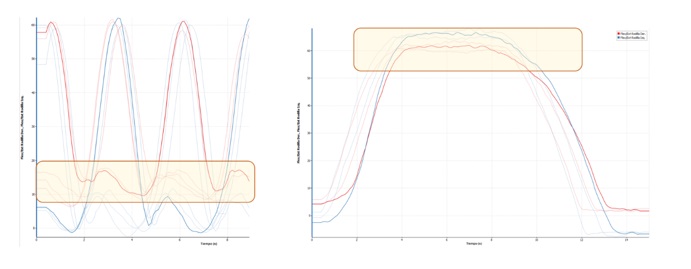
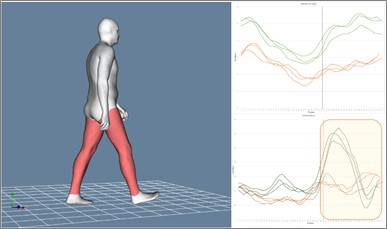
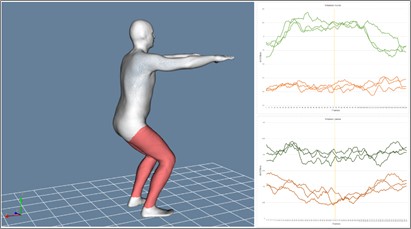
Figure 1. Joint kinematics of the operated right knee (red) and the healthy knee (blue) during gait (left) and semi-squat (right).
In general, gait functionality was normal at the kinematic level, with the exception of a slight flexion during the contact phase, which was maintained in the initial stance phase prior to swing. Additionally, during the semi-squat movement, a more or less symmetrical behaviour of the flexión angles was observed in the eccentric descent phase, with a difference of less than 5 degress.
II. STATIC MEASUREMENT OF LOWER LIMB PERIMETERS AND VOLUMES: MORPHOLOGICAL DIFFERENCES.
The direct comparison between both limbs revealed clear structural asymmetries (Figure 2), specifically:
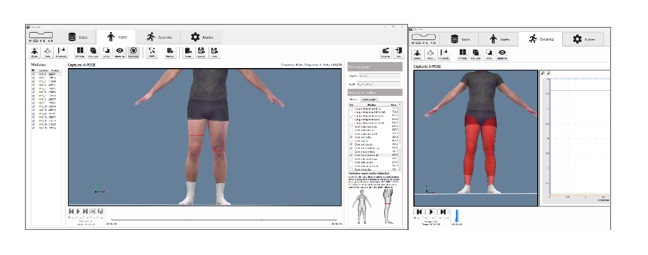
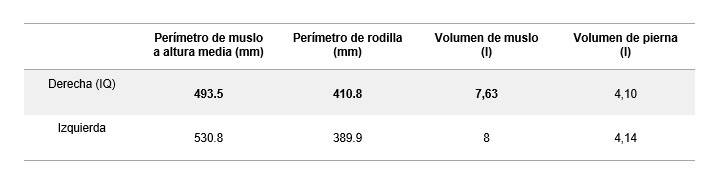
Figure 2. Static A-POSE position for calculating mid-thigh and knee perimeters (left) and thigh and leg volumes.
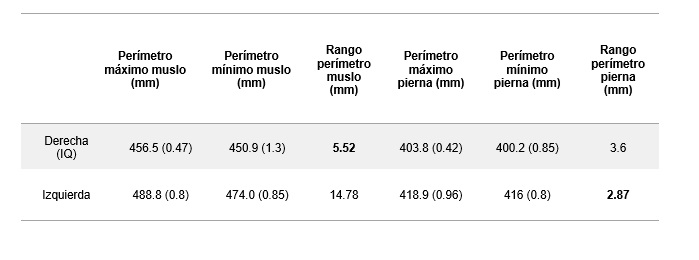
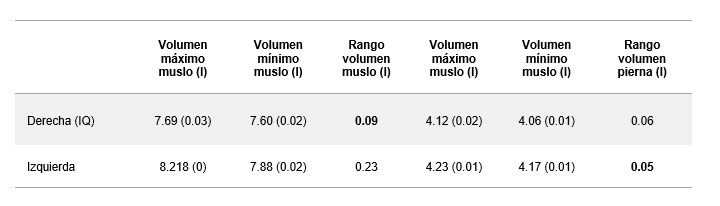
Table 1. Calculated values for mid-thigh and knee perimeters (left) and thigh and leg volumes (right) for both limbs in the static A-POSE position.
• A smaller perimeter and a reduction in volume were observed in the mid-thigh of the operated limb, consistent with muscle atrophy following the intervention and the period of load restriction.
• A larger perimeter was observed in the peripatellar region of the operated limb, consistent with possible residual oedema or inflammatory changes (Table 1).
These findings show a physiological asymmetry compared to thresholds established in large-scale anthropometric databases, such as CAESAR, where normal volumetric asymmetry in the thigh segment typically ranges between 3% and 5% [9]. In this case, the 4.6% volume deficit in dominant lower limb thigh, combined with a 3.7 cm difference in circumference, suggests a state of muscular atrophy. Consequently, this static assessment reflected a morphological asymmetry between limbs that provides an objective starting point for the subsequent dynamic functional interpretation.
III. MEASUREMENT OF DYNAMIC PERIMETERS AND VOLUMES DURING GAIT.
Below are the results related to leg and thigh perimeters during the gait cycle:
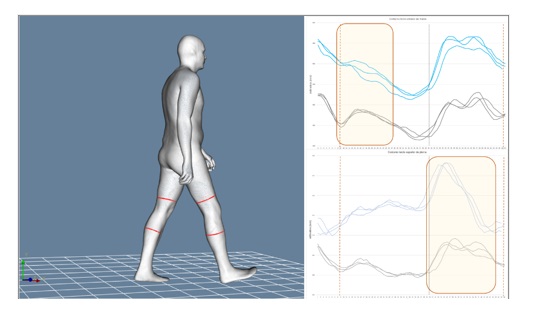
Figure 3. Dynamic perimeters of the lower third of the thigh (top right) and the upper third of the leg (bottom right) for both limbs during the gait cycle (blue: left/black: right).
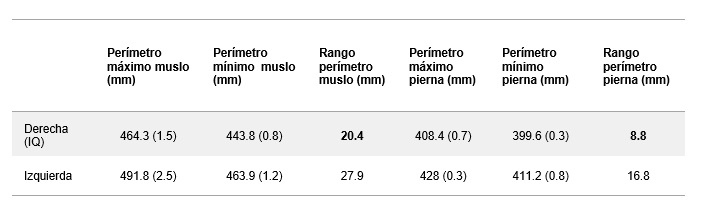
Table 2. Mean values and standard deviation of maximum, minimum, and dynamic range perimeters of the lower third of the thigh and the upper third of the leg for both lower limbs during gait.
The following are the results related to leg and thigh volumes during the gait cycle:
Figure 4. Dynamic thigh volumes (top right) and leg volumes (bottom right) for both limbs during gait cycles (green: left /orange: right)
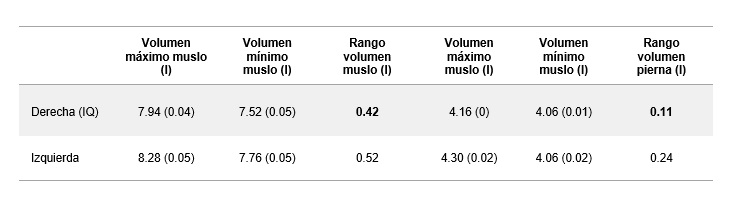
Table 3. Mean values of maximums, minimums, range, and standard deviation of maximum and minimum thigh and leg volumes for both lower limbs during the gait cycle.
The gait assessment revealed significant morphological differences between both limbs, the most relevant being:
• A different deformation pattern was observed between the two limbs for both thigh and leg perimeter during the initial loading and stance phases, as well as the swing phase (Figure 3).
• The perimeter amplitude was generally smaller in the operated limb compared to the healthy one (Table 2).
• Significant differences were observed in leg volume during the take-off and swing phases of the injured limb compared with the contralateral limb (Figure 4).
• The magnitude of the differences in dynamic thigh and leg perimeters and volumes during the execution of the movement remained in the same proportion as those observed in the static assessment (Tables 2 and 3).
• The registers are highly repeatable for perimeters and volumes.
The findings obtained from the morphological analysis described above suggest a reduced involvement of the injured limb in controlling the stance and take-off phases, consistent with the kinematic behaviour previously observed.
The overall difference indicates that, although gait was functional, soft tissue dynamics are not yet normalized compared to the healthy limb.
IV. MEASUREMENT OF DYNAMIC CIRCUMFERENCES AND VOLUMES DURING THE SEMI-SQUAT GESTURE.
The following are the results related to leg and thigh perimeters during the semi-squat cycle:
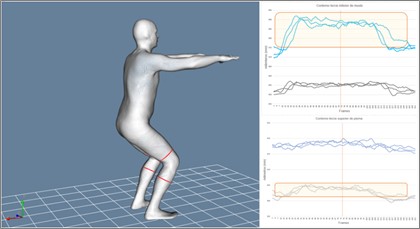
Figure 5. Dynamic perimeters of the lower third of the thigh (top right) and the upper third of the leg (bottom right) for both limbs during the semi-squat (blue: left/black: right).
Table 4. Mean values of maximum perimeters, minimum perimeter, amplitude, and standard deviation of the dynamic perimeters of the lower third of the thigh and the upper third of the leg for both lower limbs during the semi-squat.
Below are the results related to leg and thigh volumes during the semi-squat cycle:
Figure 6. Dynamic thigh volumes (top right) and leg volumes (bottom right) for both limbs during the semi-squat (green: left/orange: right).
Table 5. Mean volues of maximums, minimums, range, and standard deviation of maximum and minimum thigh and leg volumes for both lower limbs during the semi-squat cycle.
The comparison of both limbs during the semi-squat movement made it possible to identify more clearly the differences in muscle demand and postural control, highlighting:
- A deformation pattern of the injured limb different from that of the healthy limb was observed, both in perimeter values and in thigh and leg volumes (Tables 4 and 5).
These differences may indicate an increased load and activity in the thigh of the healthy side during the eccentric phase of the movement, as well as stabilization through the injured leg (Figures 5 and 6), even when the kinematic knee flexion values do not differ by more than 5 degrees.
This comparison showed that functional deficits were more noticeable in tasks with high eccentric demand and load, where the injured limb does not reproduce the same loading pattern as the healthy one.
V. ASSESSMENT OVERALL SUMMARY
The overall summary of the analysis of this case study presents the following main findings:
- The structural assessment shows that the injured limb presents greater atrophy and morphological changes that are not present in the healthy side, common finding in the 3-month post-ACL reconstruction phase.
- In the assessment of gait function, differences in morphology and magnitude of both perimeters and volumes are observed in the thigh and leg of the injured limb, which may represent functional deficits such as compensatory strategies.
- During the execution of the semi-squat movement, the differences between limbs become amplified, revealing reduced eccentric capacity and protective strategies in the injured limb that are not present in the healthy limb.
Thus, the morphological analysis reveals persistent differences in soft-tissue volume and deformation, consistent with the state of muscle function, together with the kinematic recordings, providing additional information on muscle behaviour during the phases of the studied movements.
This bilateral comparison in this case allows the identification of structural and functional deficits in movement patterns of varying demand, which may persist for months or years after surgery.
These findings are consistent with the evidence reported in the literature, where it is noted that, on the one hand, the restoration of a symmetrical gait pattern does not necessarily imply a complete recovery of muscle function; and on the other hand, that these changes have been shown to directly influence gait mechanics in more demanding tasks, such as descents or accelerations, providing evidence of a clear relationship between muscle morphology and function.
In this context, emerging technologies such as 4D dynamic surface scanning—capable of quantifying superficial deformation—offer an innovative opportunity to complement post-ACL functional evaluation. Although this line of research is still in its early stages, the analysis of soft-tissue deformation may provide additional information on the true neuromuscular state, allowing the detection of asymmetries and deficits not readily identifiable during gait or other functional tasks. Thus, integrating these tools with traditional methods may enhance diagnostic sensitivity and guide more precise decisions regarding functional progression and a safe return to sports or work activity.
CONCLUSIONS
The overall summary of the analysis of this case study presents the following main findings:
- The structural assessment shows that the injured limb presents greater atrophy and morphological changes that are not present in the healthy side, common finding in the 3-month post-ACL reconstruction phase.
- In the assessment of gait function, differences in morphology and magnitude of both perimeters and volumes are observed in the thigh and leg of the injured limb, which may represent functional deficits such as compensatory strategies.
- During the execution of the semi-squat movement, the differences between limbs become amplified, revealing reduced eccentric capacity and protective strategies in the injured limb that are not present in the healthy limb.
Thus, the morphological analysis reveals persistent differences in soft-tissue volume and deformation, consistent with the state of muscle function, together with the kinematic recordings, providing additional information on muscle behaviour during the phases of the studied movements.
This bilateral comparison in this case allows the identification of structural and functional deficits in movement patterns of varying demand, which may persist for months or years after surgery.
These findings are consistent with the evidence reported in the literature, where it is noted that, on the one hand, the restoration of a symmetrical gait pattern does not necessarily imply a complete recovery of muscle function; and on the other hand, that these changes have been shown to directly influence gait mechanics in more demanding tasks, such as descents or accelerations, providing evidence of a clear relationship between muscle morphology and function.
In this context, emerging technologies such as 4D dynamic surface scanning—capable of quantifying superficial deformation—offer an innovative opportunity to complement post-ACL functional evaluation. Although this line of research is still in its early stages, the analysis of soft-tissue deformation may provide additional information on the true neuromuscular state, allowing the detection of asymmetries and deficits not readily identifiable during gait or other functional tasks. Thus, integrating these tools with traditional methods may enhance diagnostic sensitivity and guide more precise decisions regarding functional progression and a safe return to sports or work activity.
BIBLIOGRAphy
[1] Dutaillis B, Maniar N, Opar DA, Hickey JT, Timmins RG. Lower Limb Muscle Size after Anterior Cruciate Ligament Injury: A Systematic Review and Meta-Analysis. Sports Med. 2021 Jun;51(6):1209-1226. doi: 10.1007/s40279-020-01419-0.
[2] Owen, M.K., Richardson, L., Johnson, D.L. et al. Alterations in whole muscle quality and physiological cross-sectional area measured with quantitative MRI following ACL injury. J Transl Med 23, 79 (2025). https://doi.org/10.1186/s12967-024-05980-4.
[3] Lewek, M., Rudolph, K., Axe, M., & Snyder-Mackler, L. (2002). Quadriceps femoris muscle weakness and articulation during gait after ACL reconstruction. Clinical Biomechanics, 17(8), 604–614.
[4] Hart, H. F., Culvenor, A. G., Collins, N. J., & Crossley, K. M. (2016). Knee kinematics and joint moments during gait following anterior cruciate ligament reconstruction: A systematic review and meta-analysis. British Journal of Sports Medicine, 50(10), 597–612.
[5] Klepser A, Morlock S. 4D Scanning – Dynamic View on Body Measurements. 2020 Sep. 21;1(1):30-8. https://doi.org/10.25367/cdatp.2020.1.p30-38.
[6] Basso Della-Vedova, F., De Rosario, H., Belda-Lois, JM., Porcar-Seder, R. (2024). Deformation of Skin in 4D Scans as an Indicator of Muscular Activity Compared to EMG in Biceps Contraction. In: Pons, J.L., Tornero, J., Akay, M. (eds) Converging Clinical and Engineering Research on Neurorehabilitation V. ICNR 2024. Biosystems & Biorobotics, vol 32. Springer, Cham. https://doi.org/10.1007/978-3-031-77584-0_69.
[7] Ana V. Ruescas-Nicolau, Helios De Rosario, Eduardo Parrilla Bernabé, M.-Carmen Juan, Positioning errors of anatomical landmarks identified by fixed vertices in homologous meshes, Gait & Posture, Volume 108, 2024, Pages 215-221, ISSN 0966-6362, https://doi.org/10.1016/j.gaitpost.2023.11.024.
[8] Ana V. Ruescas Nicolau, Helios De Rosario, Fermín Basso Della-Vedova, Eduardo Parrilla Bernabé, M.-Carmen Juan, Juan López-Pascual, Accuracy of a 3D temporal scanning system for gait analysis: Comparative with a marker-based photogrammetry system, Gait & Posture, Volume 97, 2022, Pages 28-34, ISSN 0966-6362, https://doi.org/10.1016/j.gaitpost.2022.07.001.
[9] De Rosario, H., Scataglini, S., Basso, F., Alemany, S., Saeys, W., Truijen, S. (2023). Applications of Using 4D Scanning Technologies in Biomechanics. In: Scataglini, S., Harih, G., Saeys, W., Truijen, S. (eds) Advances in Digital Human Modeling . DHM 2023. Lecture Notes in Networks and Systems, vol 744. Springer, Cham. https://doi.org/10.1007/978-3-031-37848-5_11
AUTHOR’S AFFILIATION
Instituto de Biomecánica de Valencia
Universitat Politècnica de València
Edificio 9C. Camino de Vera s/n
(46022) Valencia. Spain
*UMIVALEACTIVA
HOW TO CITE THE ARTICLE
Author/s: Salvador Pitarch Corresa, Fermín Basso Della Vedova, Paqui Peydro De Moya, Juan López Pascual, Eduardo Pérez Bocanegra. (20 December 2025). «Dynamic Body Surface Analysis for Functional ACL Assessment: An innovative perspective”. Revista de Biomecánica nº 72.

The publication of this article is funded by Budget Line S1048, “Technology Centres of the Valencian Community. Targeted support”, of the Valencian Regional Government’s 2025 Budget (IMAMCA/2025/7).